Ringing in the ears isn’t “just stress.” A structured ENT assessment can clarify next steps.
You’ve been hearing it for weeks. A high-pitched tone that won’t quit. A low hum that’s loudest at night when you’re trying to sleep. Someone tells you it’s just stress — and maybe you’ve started to believe them. But tinnitus, the perception of sound without an external source, is not a trivial complaint. It is a symptom that deserves a structured evaluation. And when approached properly, that evaluation can offer clarity, direction, and in many cases, real relief.
Tinnitus is not a disease. It is a symptom — a signal that something along the auditory pathway is not functioning as it should. That “something” can range from earwax buildup to age-related hearing loss, medication side effects, or stress-induced changes in how the brain processes sound.
Two broad categories exist. Subjective tinnitus — by far the most common — is sound only you can hear, generated by abnormal neural activity. Objective tinnitus is rare, produced by actual vascular or muscular activity near the ear that an examiner can sometimes detect. The distinction matters because the assessment and management of each are quite different.
Every good evaluation begins with a thorough conversation. A well-trained ENT will explore the nature of the sound (tone, hiss, pulsing, clicking), whether it’s in one or both ears, what triggers or worsens it, and what other symptoms accompany it. The presence of hearing loss, ear fullness, or dizziness alongside tinnitus significantly shapes the diagnostic picture — that triad, for instance, points strongly toward Ménière’s disease.
Your medication history matters too. Certain drugs — high-dose aspirin, some antibiotics, chemotherapy agents — are ototoxic and can damage the inner ear. Noise exposure history, head trauma, and cardiovascular conditions all add important context.
The ENT will examine the ear canal and eardrum directly using otoscopy, looking for earwax obstruction (one of the most common and easily reversible causes), signs of infection, eardrum perforation, or middle ear pathology. When pulsatile tinnitus is present, the clinician may also listen to the neck and ear area with a stethoscope to detect a bruit — an abnormal vascular sound suggesting a circulatory origin.
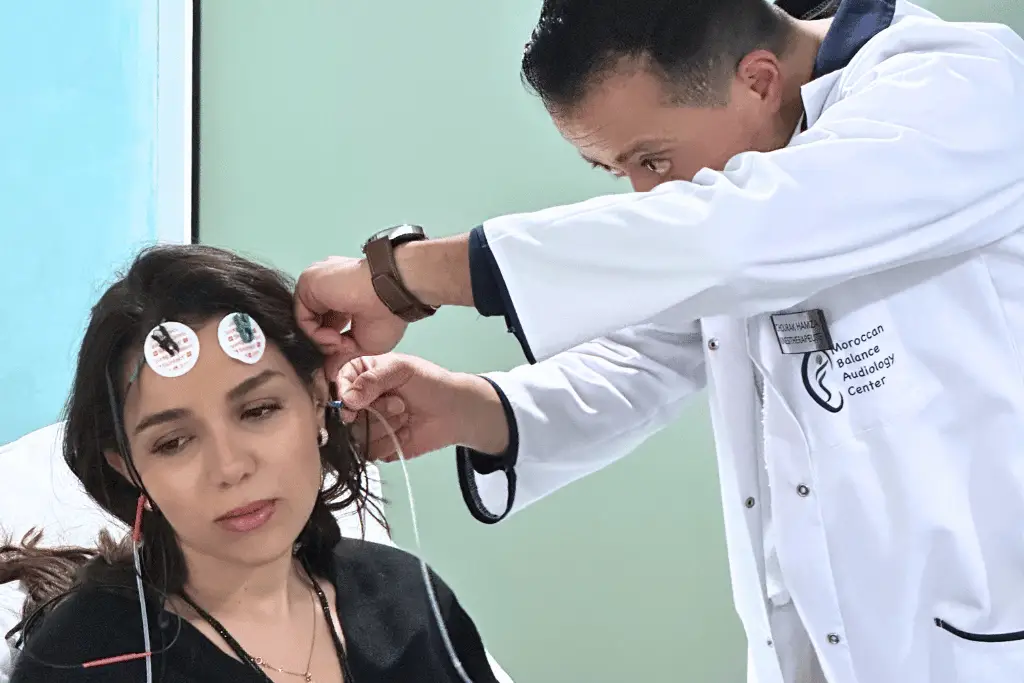
This is the most important technical component of any tinnitus evaluation. Up to 90% of people with chronic tinnitus have some degree of hearing loss — often without realizing it. A full audiological workup makes that relationship visible.
Pure tone audiometry maps your hearing thresholds across frequencies. A notch at 4,000 Hz is a classic marker of noise-induced damage. Speech audiometry tests comprehension, not just detection. Tympanometry evaluates eardrum mobility and middle ear function. Otoacoustic emissions (OAEs) can detect cochlear damage even when standard thresholds appear normal — a key tool for catching early inner ear dysfunction.
Some evaluations go further with tests designed to characterize the tinnitus itself. Pitch matching identifies which frequency most closely resembles what you hear. Loudness matching reveals how loud it actually is — most people are surprised to find their tinnitus matches tones only 5 to 10 decibels above their hearing threshold, remarkably soft yet subjectively overwhelming. Minimum masking level testing informs whether sound therapy or hearing aids are likely to help.
Tinnitus is not experienced in the ear alone — it lives in your sleep, your concentration, your relationships. A responsible evaluation includes validated questionnaires such as the Tinnitus Handicap Inventory (THI), which measures functional and emotional impact across 25 items. Scales for anxiety, depression, and sleep quality are equally relevant. Research consistently shows that psychological factors — particularly anxiety and hypervigilance to sound — strongly predict who develops debilitating tinnitus. Addressing them is central to any management plan.
Not every case requires imaging, but some presentations do. MRI of the internal auditory canals is indicated for unilateral tinnitus with asymmetric hearing loss, primarily to exclude an acoustic neuroma — a rare but important diagnosis. CT scanning evaluates bony temporal bone structures. Doppler ultrasound or CT angiography may be requested when a vascular cause is suspected. Blood tests can rule out thyroid dysfunction, anemia, or autoimmune conditions that affect inner ear function.
Consider booking a consultation if the sound has lasted more than two weeks, appears in one ear only, pulses with your heartbeat, comes with hearing loss or dizziness, or is affecting your sleep and daily functioning. The earlier a reversible cause is caught, the better — and early assessment prevents tinnitus from becoming entrenched in the nervous system before any intervention begins.
Tinnitus is a symptom with a biology, a variability, and a structured path forward. A proper ENT assessment can transform a vague, distressing complaint into an understood, manageable condition. You don’t have to just live with it — but you do have to start by getting it properly evaluated.
Post Tags :
Share :

Clarity and care for vertigo, balance, hearing, and sleep symptoms.
Copyright © 2026 by Keshrise